Transforming Newborn Care in Rural Uganda
“One mother came back for review yesterday, you should have seen the smile on her face. Her baby was 1.1kg at birth. In two months, the baby is now 2.2kgs”, says Zabia Hamba, the pride in her voice palpable.
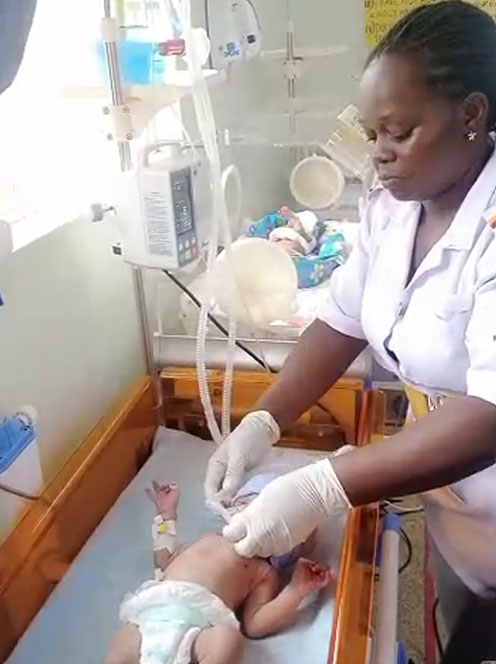
Zabia, a midwife in her late thirties, continues to speak softly as she gently places a tiny, sleeping baby back into an incubator. The soft hum of different machines merges with the distant murmur of mothers chatting outside the Neonatal Intensive Care Unit (NICU).
“This baby you see here is two years old, but was brought in at 0.9 grams, the mother was in tears”, she says, “but look at her now, she’s thriving. Her face is glowing, and there is a newfound radiance on her skin. You should see how delighted the parents are right now”, she smiles softly.
Yet Zabia is quick to note that before Bulamu Healthcare set up this NICU, the gentle kicks of recovering babies and the cheerful chatter of waiting mothers were not always part of the scene at Budaka Health Center IV, nestled in the small township of Budaka in Eastern Uganda.
A couple of years prior, the cry of a newborn in distress at the facility was met with a heavy sense of fear and helplessness; the only hope was a 31-mile journey further east to Mbale Regional Referral Hospital.
“We used to refer all newborns who needed special attention to Mbale. Every single one of them,” Zabia recalls. “Even the most minor cases. Because most of us had huge knowledge gaps. We didn’t know much to do with newborn care beyond delivering”.
This referral system was a heavy burden. For families, it meant crippling transport costs and anxious days away from home. For babies, the journey could be fatal. And for the overwhelmed NICU in Mbale, the constant influx from surrounding districts meant dangerous congestion.
This absence of essential expertise and functional equipment meant Budaka could not adequately care for newborns. The facility had a single incubator, but it stood as a symbol of their limitations.
“We didn’t know anything about it,” Zabia admits, “so we would just switch it on and put the babies there. When Bulamu came, we realized we were putting the babies on dry oxygen. We didn’t even know we had to put distilled water in the humidifier ”, she laughs.
But today, that’s a totally different picture. At the start of 2024, Bulamu established a fully functional NICU at the facility with a 20-bed capacity. The impact was immediate and profound, currently saving nearly 100 fragile newborns every month. This NICU is one of twelve Bulamu has either set-up or upgraded in different government health facilities around the country.
“The community is very happy now that instead of going to Mbale, the services are available here”, Zabia says, “Families no longer endure long, costly journeys, and babies get immediate, life-saving expert care close to home.”
“We have also decongested the Mbale Referral”, she says, “Some facilities now refer babies here. We get newborns from neighboring districts like Kibuku, Butebo, Butaleja, and Namutumba”.
“We also follow up on our babies. After discharge, we go out to the community at least once a month to see how they are doing”, she adds proudly.
This amazing transformation began with knowledge and empowerment.
“They trained us”, she says, “they gave us comprehensive knowledge on Neonatal Care, taught us how to use the equipment, and created a skills lab so that we could pass on that knowledge to more healthcare professionals from here and beyond.”
“As a facility, I cannot tell you enough how happy we are. And personally, the gratitude even goes beyond that. I now have such commendable knowledge of the NICU, I feel like an expert”, says Zabia, who is now the district mentor at the skills lab established by Bulamu.
Twice a month, along with the other health workers she received training with, they train midwives from lower-level facilities, and quarterly, they go to those facilities for follow-up mentorship.
Bulamu’s support for these facilities also extends to vital supplies such as midwife and mama kits, easing the burden on mothers who arrive at the hospital without essentials.
“Many times we have mothers who come completely without anything, and it’s not because they are stubborn; they just do not have the money to buy those essentials. If you look at such a mother, you feel her pain”, Zadia says, “But now with these supplies from Bulama, such mothers are catered for”.
Beyond the physical tools, the facility has also been capacitated to use data to track performance and inform decisions. To this effect, Bulamu set up a matrix board at the NICU. This data-driven approach allows them to identify trends, retrain staff, and improve protocols, continuously enhancing the quality of care.
“For example, if in a month we have say 25 birth infection cases, we sit and discuss. Where is it coming from? Is it the mothers? The midwives? Is the ward not well cleaned? We come up with resolutions. If it is birth asphyxia, then we go back to our midwives and find a way to address it.”
Zabia says the collaborative and encouraging approach of the Bulamu team had a lasting impact on them, transforming not just the hospital’s operations but also the staff’s personal and professional skills, inspiring a new philosophy of leadership.
“I really like the Bulamu team. They have been very patient with us throughout the learning process. In the beginning, we were very disorganized, but not once did they say, ‘Oh, these people, we are tired of them.’ Whenever they come, they encourage us ‘Now, let’s do this, let’s do this.’ That inspired me. This gentle guidance taught me to lead with empathy, creating a lasting culture of resilience and kindness that continues to drive success in the Skills lab,” she says.
“One mother came back for review yesterday, you should have seen the smile on her face. Her baby was 1.1kg at birth. In two months, the baby is now 2.2kgs”, says Zabia Hamba, the pride in her voice palpable.
Zabia, a midwife in her late thirties, continues to speak softly as she gently places a tiny, sleeping baby back into an incubator. The soft hum of different machines merges with the distant murmur of mothers chatting outside the Neonatal Intensive Care Unit (NICU).
“This baby you see here is two years old, but was brought in at 0.9 grams, the mother was in tears”, she says, “but look at her now, she’s thriving. Her face is glowing, and there is a newfound radiance on her skin. You should see how delighted the parents are right now”, she smiles softly.
Yet Zabia is quick to note that before Bulamu Healthcare set up this NICU, the gentle kicks of recovering babies and the cheerful chatter of waiting mothers were not always part of the scene at Budaka Health Center IV, nestled in the small township of Budaka in Eastern Uganda.
A couple of years prior, the cry of a newborn in distress at the facility was met with a heavy sense of fear and helplessness; the only hope was a 31-mile journey further east to Mbale Regional Referral Hospital.
“We used to refer all newborns who needed special attention to Mbale. Every single one of them,” Zabia recalls. “Even the most minor cases. Because most of us had huge knowledge gaps. We didn’t know much to do with newborn care beyond delivering”.
This referral system was a heavy burden. For families, it meant crippling transport costs and anxious days away from home. For babies, the journey could be fatal. And for the overwhelmed NICU in Mbale, the constant influx from surrounding districts meant dangerous congestion.
This absence of essential expertise and functional equipment meant Budaka could not adequately care for newborns. The facility had a single incubator, but it stood as a symbol of their limitations.
“We didn’t know anything about it,” Zabia admits, “so we would just switch it on and put the babies there. When Bulamu came, we realized we were putting the babies on dry oxygen. We didn’t even know we had to put distilled water in the humidifier ”, she laughs.
But today, that’s a totally different picture. At the start of 2024, Bulamu established a fully functional NICU at the facility with a 20-bed capacity. The impact was immediate and profound, currently saving nearly 100 fragile newborns every month. This NICU is one of twelve Bulamu has either set-up or upgraded in different government health facilities around the country.
“The community is very happy now that instead of going to Mbale, the services are available here”, Zabia says, “Families no longer endure long, costly journeys, and babies get immediate, life-saving expert care close to home.”
“We have also decongested the Mbale Referral”, she says, “Some facilities now refer babies here. We get newborns from neighboring districts like Kibuku, Butebo, Butaleja, and Namutumba”.
“We also follow up on our babies. After discharge, we go out to the community at least once a month to see how they are doing”, she adds proudly.
This amazing transformation began with knowledge and empowerment.
“They trained us”, she says, “they gave us comprehensive knowledge on Neonatal Care, taught us how to use the equipment, and created a skills lab so that we could pass on that knowledge to more healthcare professionals from here and beyond.”
“As a facility, I cannot tell you enough how happy we are. And personally, the gratitude even goes beyond that. I now have such commendable knowledge of the NICU, I feel like an expert”, says Zabia, who is now the district mentor at the skills lab established by Bulamu.
Twice a month, along with the other health workers she received training with, they train midwives from lower-level facilities, and quarterly, they go to those facilities for follow-up mentorship.
Bulamu’s support for these facilities also extends to vital supplies such as midwife and mama kits, easing the burden on mothers who arrive at the hospital without essentials.
“Many times we have mothers who come completely without anything, and it’s not because they are stubborn; they just do not have the money to buy those essentials. If you look at such a mother, you feel her pain”, Zadia says, “But now with these supplies from Bulama, such mothers are catered for”.
Beyond the physical tools, the facility has also been capacitated to use data to track performance and inform decisions. To this effect, Bulamu set up a matrix board at the NICU. This data-driven approach allows them to identify trends, retrain staff, and improve protocols, continuously enhancing the quality of care.
“For example, if in a month we have say 25 birth infection cases, we sit and discuss. Where is it coming from? Is it the mothers? The midwives? Is the ward not well cleaned? We come up with resolutions. If it is birth asphyxia, then we go back to our midwives and find a way to address it.”
Zabia says the collaborative and encouraging approach of the Bulamu team had a lasting impact on them, transforming not just the hospital’s operations but also the staff’s personal and professional skills, inspiring a new philosophy of leadership.
“I really like the Bulamu team. They have been very patient with us throughout the learning process. In the beginning, we were very disorganized, but not once did they say, ‘Oh, these people, we are tired of them.’ Whenever they come, they encourage us ‘Now, let’s do this, let’s do this.’ That inspired me. This gentle guidance taught me to lead with empathy, creating a lasting culture of resilience and kindness that continues to drive success in the Skills lab,” she says.
“We are very grateful for the support from all the donors behind this. They have made our work easy and enjoyable as health workers”.
Name:
Zabia
Treatment:
Maternal and Newborn Health
Year:
2025

You can help ensure a better future for Ugandans in need by becoming a lifeline today.
Help save a newborn like Miracle.
Access to quality healthcare is everything. But our work to bring lifesaving treatments to Africans most in need can’t start without your support. You can help provide emergency transportation, crucial medical supplies, essential training, and hope. No matter how much you choose to give, your gift will help fund affordable healthcare and training for those who need it most.
